-2 NK (Natural Killer) Cells and Immunity
페이지 정보

본문
Let’s learn about immunity.
Immunity is important for patients, especially cancer patients. Do cancer patients also need NK (Natural Killer) Cells? Of course you need it. In general, NK (Natural Killer) Cell is known to be useful for blood cancer, which is a non-solid cancer, but is somewhat less effective for solid cancer (cancer that forms hard lumps, including most cancers such as stomach cancer and breast cancer). However, Panacell Biotech is researching It is one of the very few institutions that can culture and perform the necessary cells for adult patients with a single injection through simultaneous culture of NK cells and NK-T cells. As cancer progresses or is undergoing chemotherapy, the immune system decreases to zero. What is important in this case is the number of cells. Therefore, culturing ability is important.
Panacell Biotech is an organization that has received a cell processing facility permit from the Ministry of Food and Drug Safety.
In addition, Panacell Biotech is researching Car-NK and Car-Macrophage to treat solid tumors.
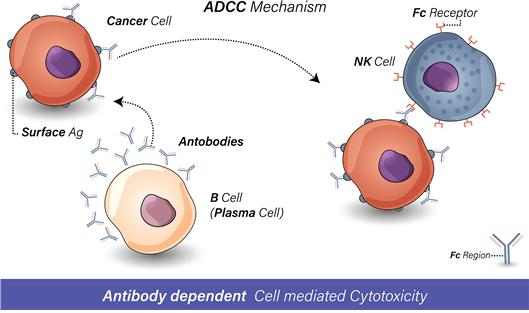
1. The impact of adipose-derived stem cells (ADSC) on immunity.
1. What is immunity?
Immunity, in English, is immunity, and in Chinese characters, it means ‘avoiding adverse effects.’ Station means plague, but it means ‘avoiding plague.’ To explain it further, immunity refers to the action or state of killing or neutralizing pathogens against infection or disease.
Immunity includes innate immunity and acquired immunity. As the name suggests, innate immunity is the immune system we already have at birth. For example, our skin and the mucous membranes in our mouths function to prevent the invasion of pathogens, so they are innate immunity. On the other hand, acquired immunity is the immune system that our body develops when it comes into contact with pathogens after birth, and lymphocytes are involved. All cases involving so-called antibodies can be thought of as acquired immunity.
2. What are the cells involved in immunity?
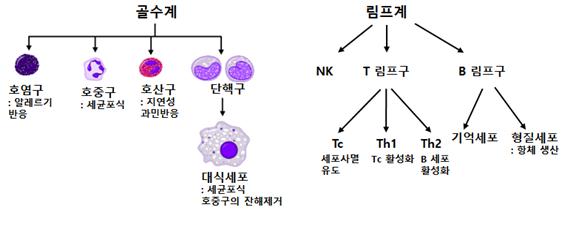
In short, they are white blood cells. Exceptionally, dendritic cells that reside only in tissues are also responsible for immunity. White blood cells can be broadly divided into the myeloid system and the lymphoid system. White blood cells belonging to the myeloid system include neutrophils, eosinophils, basophils, and monocytes, and white blood cells belonging to the lymphatic system include B lymphocytes, T lymphocytes, and natural killer (NK) cells. When activated, monocytes differentiate into macrophages and are responsible for ingesting pathogens, B lymphocytes are cells that produce antibodies, and T lymphocytes activate B lymphocytes or differentiate into Tc cells to kill virus-infected cells or cancer cells. Perform.
3. How do adipose-derived stem cells, or ADSCs, affect immunity?
If the immune function is excessive, it plays a role in suppressing the immune function, and if the immune function is insufficient, it promotes the immune function. In other words, it can be thought of as playing a role in balancing immunity.
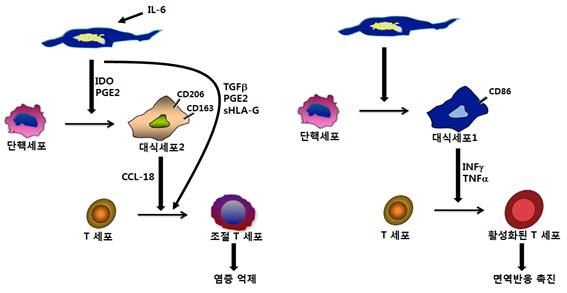
It is known that this immunomodulatory effect of ADSC is due to the control of macrophage polarization and the action of the enzyme IDO (indoleamine 2,3-dioxygenase) expressed by ADSC (Bernardo and Fibbe, Cell Stem Cell 13, October 3, 392 ~402, 2013; Luk et al., Front. Immunol. 2017, 8:1042). ADSCs exposed to IL-6 produced by the inflammatory response produce IDO and prostaglandin E2 (PGE2), which activates monocytes into macrophages 2. Macrophage 2 and ADSC play a role in suppressing inflammatory responses by differentiating T cells into regulatory T cells (Treg). On the other hand, ADSCs that are not exposed to IL-6 due to lack of inflammatory response activate monocytes into macrophages 1. Macrophage 1 plays a role in promoting immune responses by activating T cells into Tc cells and Th cells.
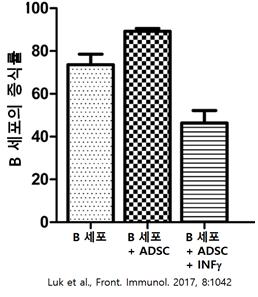
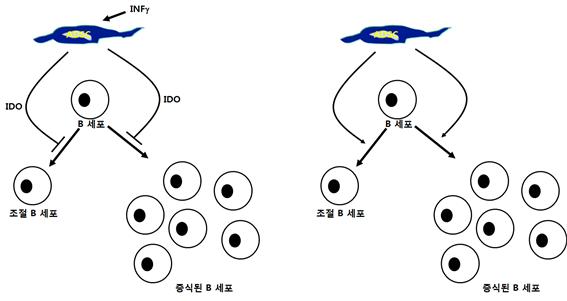
The immunomodulatory effect by ADSCs is also seen in the regulation of B cells. When there is no inflammatory response, ADSC promotes the proliferation of B cells and plays a role in inducing regulatory B cells, preparing the immune response to occur immediately. On the other hand, when an inflammatory response exists, ADSCs are activated by interferon gamma (INFγ) to produce IDO, and IDO inhibits the proliferation and maturation of B cells by depleting tryptophan (Luk et al., Front. Immunol. 2017, 8 :1042).
4. What clinical effects can immunomodulation by ADSC have?
It can be expected to have a wide range of therapeutic effects on diseases caused by immune abnormalities, and in fact, various therapeutic effects have been reported. Let me introduce you to just a few of them. Systemic sclerosis is a type of autoimmune disease in which the area around the mouth hardens and gradually becomes difficult to open the mouth. To treat scleroderma around the mouth, the patient's ADSC and PRP were injected around the mouth, allowing the patient to open the mouth wider (Virzì et al. Stem Cell Research & Therapy (2017) 8:236).
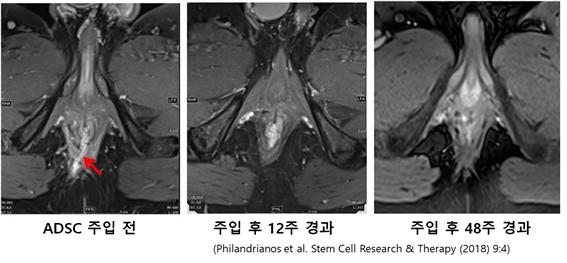
Crohn's disease is a chronic inflammatory disease that affects the digestive epithelium from the mouth to the anus, and perianal fistulas appear in almost one-third of Crohn's disease patients. To treat this fistula, surgery and drug treatment are combined, but it is known to be quite difficult to treat. After suturing the hole on the rectal side of the perianal fistula, ADSC-microfat mixture was injected around the wall of the perianal fistula, and as a result of observation, it was observed that the fistula disappeared after 12 weeks, and the fistula disappeared for 48 weeks. No abnormalities were observed (Philandrianos et al. Stem Cell Research & Therapy (2018) 9:4).
In addition to these effects, ADSC is known to be effective in diseases caused by immune disorders such as atopy, psoriasis, rheumatoid arthritis, and autoimmune epilepsy.
- PrevWharton Jelly Stem Cells 24.04.16
- Nextwhat is an exosome? 24.04.16
댓글목록
등록된 댓글이 없습니다.





 +82-32-252-3210
+82-32-252-3210 info@panacellbio.com
info@panacellbio.com 3F, Inspire Ent. Resort, 127 Jung-gu, Incheon, Republic of Korea
3F, Inspire Ent. Resort, 127 Jung-gu, Incheon, Republic of Korea